Total Hip Anterior Approach
GENERAL INFORMATION ON HIP REPLACEMENT SURGICAL APPROACH AND REHAB AFTER SURGERY.
Total Hip Replacement is an extremely successful surgical procedure to improve a patient’s quality of life when arthritic hip pain becomes debilitating.
Hip replacement surgery offers patients the ability to return to their daily (and some sporting) activities without pain and with improvement in hip flexibility and movement. Patients with a significant limp as a result of an arthritic hip will often walk normally again after recovering from surgery.
The timing of surgery is a quality of life decision and it is never to late to replace the hip joint provided one’s general health is satisfactory.
There are various approaches that surgeons use to replace the arthritic hip.
All recognized surgical approaches work. Using tried and tested Hip Replacement designs, there is more evidence now that suggests a hip replacement may well last most patients’ lifetimes.
The Australian Joint Replacement Registry and many publications show clear data confirming that more experienced surgeons have better patient outcomes.
The most important factor in determining long-term success of a hip replacement is to choose a skilled surgeon and be guided by his/her recommendations.
Every patient would like to recover as quickly as possible with as little pain as possible. Surgical and Anaesthetic techniques have improved significantly and these improved techniques have allowed an easier and faster recovery.
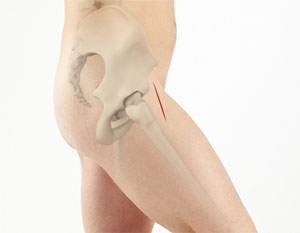
The Minimally Invasive Direct Anterior Approach (often termed DAA or AMIS) is an approach that may lend itself to a quicker short-term recovery due to the fact that the surgical approach uses intermuscular planes allowing exposure of the hip joint without detaching muscle off bone. This may allow the patient the ability to recover quicker and return to function quicker compared to other approaches.
There are many published articlesthat report that the anterior approach usually leads to a quicker short term recovery HOWEVER all published articles also confirm that after 6-12 months patients having had a successful hip replacement, function equally well no matter what approach is used.
The Australian National Joint Register 2019 publication reports that there was no difference in the overall rate of revision when surgical approach is compared
The most commonly used worldwide approach to hip surgery is the Posterior Approach (ie from the back) and published results show there is no significant difference between a well done posterior approach and well done anterior approach at 6-12 months after surgery. The posterior approach requires splitting the gluteus maximus (buttock) muscle and detachment of the short external rotator muscles and then reattachment of these muscles/capsule and hence the slightly slower recovery that may occur compared to the anterior approach.
There are some short-term hip movement restrictions in the posterior approach (internal rotation of the hip beyond 90 degrees of flexion) for 6-8 weeks to prevent hip dislocation whilst the capsule/muscle repair recovers. The anterior approach is inherently a very stable approach not requiring muscle repair and movement restriction. Patients usually can return to driving at an earlier stage (1-2 weeks) if they have had an anterior approach.
IMPORTANT INFORMATION
As an experienced hip surgeon (over 22 years performing more than 6000 hip replacements) and I am very comfortable performing either the anterior or posterior approach for the arthritic hip. My general preference is to perform the minimally invasive anterior approach unless there are contra-indications or perceived technical difficulties.
Not all patients may be suitable for the anterior approach due to many factors including:
- Morbid Obesity
- Abnormal anatomy (such as Hip Dysplasia, Perthes, previous fractures, abnormal bone structure etc.)
- Severe osteoporosis.
- Significant muscular build resulting in very tight and limited joint visualization.
- Significant leg length discrepancy.
- Deficient bone requiring bone grafting or augmentation of the socket.
- Specialised hip implants needing to replace the hip joint.
- Most revision hip surgery.
The Responsible Approach:
Every patient I see has an individual assessment taking into account their hip pathology, degree of arthritis, day to day function, general health and body habitus. I will then advise what I believe to be the best surgical approach to achieve the best clinical outcome with the least chance of complications.
Whilst I would prefer from a general recovery perspective to perform an anterior approach it is MORE IMPORTANT to ensure a safe recovery with appropriate attention to the underlying problems at hand. If I feel that the anterior approach is not suitable, I will perform a posterior approach AND will reassure the patient that whilst they may have a slightly slower recovery compared to the anterior approach, their LONG-TERM function will be identical.
Rehabilitation following Hip Replacement:
Many patients DO NOT require formal in-patient rehabilitation and can be discharged home with outpatient physiotherapy and a home-based exercise program. Studies have conclusively shown that there is NO difference in outcomes between inpatient and outpatient rehab.
There is a false perception that by not going to in-patient rehab your result will be inferior. This is simply NOT TRUE and many published studies have proven that home discharge is as good.
I encourage patients to go home following surgery however there are patients who benefit from in-patient rehab when home circumstances are not ideal or where extra medical attention is required.
The Final Word……..
The key to a successful hip replacement with the best chance of a good functional outcome and the least chance of complications is to choose an experienced skilled hip surgeon. Whilst the Anterior Approach may afford a quicker short-term recovery, not all patients are suitable for this approach, yet be reassured that at 6-12 months the posterior approach performs equally as well.
Updated April 2020
![]() General Information on the Minimally Invasive Direct Anterior Approach
General Information on the Minimally Invasive Direct Anterior Approach
You will need the Adobe Reader to view and print these documents.